Some patients with heart rhythm disturbances ("arrhythmias") do not respond adequately to treatment with medication, and for other arrhythmia patients, therapy with medications is not as safe or appropriate as more definitive treatment. Catheter ablation (a-blay-shun) is a procedure used to selectively eliminate (damage or get rid of) the heart cells causing the arrhythmia.
While many energy sources are being investigated to perform catheter ablation procedures, radiofrequency (RF) electrical energy is most commonly used today. RF energy consists of high frequency radiowaves and has been used safely during surgical procedures for many years to cauterize (burn) tissue and prevent bleeding. When delivered by catheters that are positioned inside the heart, RF energy can selectively cauterize the heart cells responsible for an abnormal heart rhythm. Catheter ablation is designed to permanently cure your arrhythmia, or if that is not possible, to make them less frequent, slower, and better tolerated.
Your heart has its own natural electrical system which makes it beat (figure 1). Normally, this electrical impulse begins in the sino-atrial (SA) node located in the upper right chamber (right atrium) of the heart. The impulse spreads across both atria causing them to contract simultaneously and squeeze blood into the lower pumping chambers (ventricles). While the atria are contracting, the electrical impulse continues through the atrio-ventricular (AV) node. The AV node is the "gate-keeper" to the lower chambers and is normally the only electrical connection between the upper and lower chambers. After a split second pause, the impulse then continues down through both of the ventricles causing them to contract and squeeze blood out to the body and lungs.
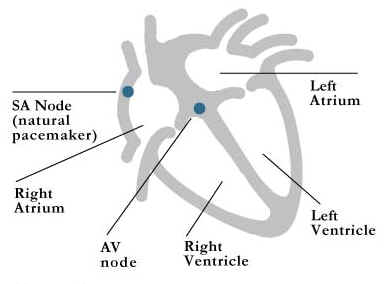
Figure 1: normal conduction system
Changes in the heart's electrical system can cause periodic episodes of an abnormal heart rhythm. When this occurs, the heart can beat very rapidly and cause symptoms of palpitations, lightheadedness or dizziness, shortness of breath, a feeling of fullness in the throat, chest pain/pressure, fatigue, or fainting. Ablation is designed to prevent your tachyarrhythmia (fast abnormal rhythm) and thereby relieve symptoms.
Heart rhythm disturbances that originate in the upper heart chambers and are referred to as supraventricular tachycardias or SVT, and as a group are the most common type of arrhythmia. These arrhythmias are generally considered benign and are not life threatening. There are five major types of rhythm disturbances that arise in the upper heart chambers: 1). AV nodal reentrant tachycardia, 2). AV reentrant tachycardia, 3). Atrial tachycardia, 4). Atrial flutter, and 5). Atrial fibrillation. Your physician and/or nurse will review with you the suspected mechanism of your SVT.
Atrial fibrillation (AF) is the most common sustained tachyarrhythmia, and generally occurs in people with underlying heart disease (figure 2). Atrial fibrillation can also occur in people without other heart problems, a condition termed “lone atrial fibrillation”. The exact mechanism of AF is still being investigated. In some patients it may be due to wandering, disorganized, electrical circuits (wavefronts) throughout the upper chambers (atria). In others, it may be caused by a single rapidly firing electrical spot (focus), which is commonly located in one of the pulmonary veins near where they empty into the left atrium.
During atrial fibrillation, the AV node is bombarded with many electrical impulses for the atria (the abnormal wavefronts), which cause the lower chambers (ventricles) to beat rapidly and irregularly.
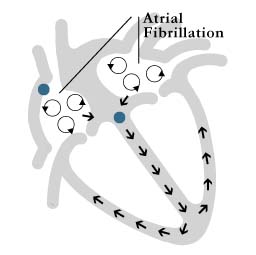
Figure 2: atrial fibrillation
Atrial Flutter is due to an electrical impulse that travels around a defined circuit in the right atrium. This impulse is funneled through a small region of heart tissue (isthmus) located at the bottom of the right atrium. Ablation will prevent any electrical impulses to pass through this region. (figure 3)
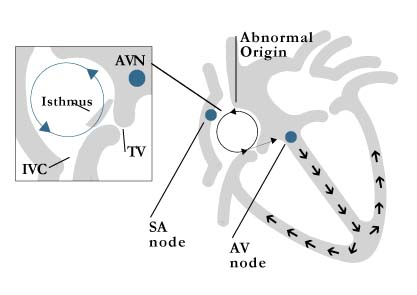
Figure 3: atrial flutter circuit and isthmus
Atrial fibrillation and atrial flutter are usually easily identified, as they have a characteristic appearance on the electrocardiogram (ECG). The other three SVTs are often harder to distinguish on an ECG. Of these, the most common SVT is “AV nodal reentrant tachycardia” (AVNRT) and originates in the area of the AV node (figure 4). This mechanism accounts for approximately 60% of all SVTs (excluding atrial fibrillation and flutter. Some people are born with 2 pathways within their AV node.). Under the right conditions an electrical impulse can rapidly travel around and around within the AV node going up one pathway and down the other. Ablation will eliminate one of the pathways thereby curing your arrhythmia.
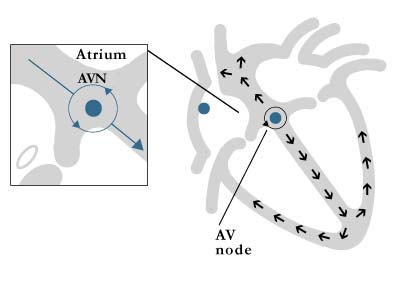
Figure 4: AV nodal reentrant tachycardia
Some people are born with an extra connection (accessory pathway) between the upper and lower chambers of the heart. When the accessory pathway is visible on the electrocardiogram (ECG) this is called the "Wolff-Parkinson-White" syndrome or "WPW". Other people may have an accessory pathway which is not visible. This is called a "concealed" (or hidden) accessory pathway. Under the right conditions an electrical impulse can travel down the normal electrical connection and then back up the accessory pathway. This is known as "AV reciprocating tachycardia (AVRT)" (figure 5). This mechanism accounts for approximately 30% of SVTs. Ablation will eliminate the accessory pathway.

Figure 5: AV reciprocating tachycardia
Atrial tachycardia is due to an abnormal electrical impulse originating from a spot (focus) in the upper chambers (atria) other than the normal pacemaker center (SA node). Ablation will eliminate this abnormal focus (figure 5).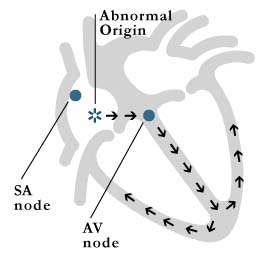
Figure 6: atrial tachycardia
Heart rhythm disturbances can also originate in the lower pumping chambers or ventricles, the most common being ventricular tachycardia (VT) (figure 7). Ventricular arrhythmias tend to be more serious than supraventricular arrhythmias and are generally life threatening. VT most often arises from areas of scar tissue in the ventricle, which is the result of a heart attack. However, VT can also occur in a normal, healthy heart. Ablation can be used to treat VT in some instances. Your physician and/or nurse can discuss this possibility with you.
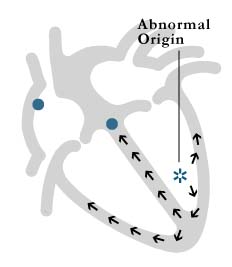
Figure 7: ventricular tachycardia
Once the decision to have an ablation is made, you will be scheduled for some routine blood work. Be sure to ask your cardiologist whether or not you should stop any of your medications before the procedure. You should also let them know if you have any allergies to medications or x-ray dye. Ablation cannot be safely performed on pregnant patients. Women who are pregnant can almost always be effectively and safely treated with other modalities until they deliver. Ablation can be considered at that time.
On the night before your ablation procedure, you cannot have anything to eat or drink after midnight. You can take your medications on the morning of the procedure with a sip of water, unless the physician or nurse has instructed you otherwise.
Upon your arrival to the Electrophysiology (EP) Lab, you will be asked to change into a hospital gown and then will be assisted onto a padded x-ray table. Your heart rate and blood pressure will be checked and you will be placed on a heart monitor. An intravenous (IV) line will be started. You will be given a mild sedative through the IV to help you relax and make you sleepy throughout the procedure.
A team of specialists including Electrophysiologists, one or more nurses, an EP technologist and a radiology technologist will perform your ablation. The members of the team will check you throughout the procedure to monitor your condition. Please do not hesitate to ask them any questions.
The procedure sites (both groin areas and sometimes the right side of your neck) will be shaved and washed with an antiseptic soap. You will then be covered from your neck to your toes with a large sterile sheet that helps to prevent infection. The Electrophysiologists will wear masks, gowns and gloves in order to maintain sterile conditions during the procedure. The lighting in the EP lab will be dimmed during most of the procedure to allow the physicians to view the heart monitors and x-ray screens more clearly.
A local anesthetic (similar to the type you receive at the dentist) will be administered at the sites chosen for insertion of the catheters (small, thin tubes). You may feel a temporary sting or slight pressure as the area is anesthetized, in addition to some pressure as the catheters are inserted. If you experience undue discomfort, please let the physician or nurse know so they can provide you with additional medicine. Once the catheters are in position, you should feel comfortable.
Before the actual ablation can be performed, the physicians must first identify the area where your abnormal rhythm is coming from. They will record the electrical activity of your heart during your abnormal rhythm to create a "map" of the precise area of heart muscle responsible. During this time you may experience some palpitations, but otherwise you will be resting quietly. Once the physicians have identified the mechanism of your abnormal rhythm, they will insert a special catheter (the one that will deliver the RF energy).
The catheter tip will be positioned against the inner surface of the heart muscle as close as possible to the site of origin of your abnormal rhythm. Radiofrequency current is then passed into the area through the tip of the catheter in order to cauterize (burn) and silence the cells responsible for your abnormal heart beat. If you experience any chest discomfort or pressure, be sure to inform the staff during the procedure. The length of the procedure is variable, but most commonly ranges between three to four hours.
Most patients experience no difficulty with the ablation procedure. However, any invasive procedure that involves the heart and blood vessels has some potential risk. The most common risks include infection or bleeding. Other risks include, but are not limited to: damage to an artery or vein, formation of a blood clot which, on rare occasions, can lead to a heart attack or stroke or travel to a lung, collapsed lung or a perforation of the heart muscle or other structures.
Ablation of certain areas of the heart may cause the heart to slow too much. This may require insertion of a permanent pacemaker. The risk of needing a permanent pacemaker is in the range of 1% or less for ablation of some arrhythmias, but virtually 0% for ablation of others. If the ablation procedure is long, the x-rays used can be irritating to the skin. The Electrophysiologist will review the risks and benefits of the ablation procedure in detail with you prior to your procedure. Please be assured that every safeguard will be provided for you before, during and after the procedure to keep the risk of any complications low.
When the procedure is finished, you will be moved to a stretcher and taken to a recovery area. Under the physician's guidance, a technician will remove the catheters and apply pressure to the sites for approximately 20 minutes. This helps to control any bleeding that may occur. Once you are stable, you will be transferred to a regular hospital room. The nurse will check your blood pressure and heart rate, and monitor the insertion sites and pulses at regular intervals. You will be able to resume your previous diet shortly after the procedure is completed and you are considered stable.
An important aspect of your care following catheter ablation involves your cooperation in remaining in bed for at least four hours following the procedure. The leg used for insertion of the catheters must remain straight and at rest so that the wound can heal properly. You will not be permitted to use the bathroom during this time and must therefore use a bedpan or urinal. If you have pain or notice any bleeding at the insertion sites, please call your nurse immediately.
The physician who performed your procedure will visit you later in the day to examine the insertion sites. If you have any questions regarding the procedure, please call your nurse or speak with the physician when they visit you. The physician may discharge you the afternoon or evening of the procedure if everything is stable. You must have someone available to drive you home and stay with you that evening. Otherwise, you will be monitored overnight and discharged the following morning. Recovery from catheter ablation is quick. After 24 hours, you should feel free to resume most of your normal activities.
Is catheter ablation safe?
Like any invasive procedure, catheter ablation has some risk associated with it. Overall, catheter ablation is considered a safe and highly effective treatment for certain heart rhythm disturbances. You should discuss the relative risks and benefits of the procedure with your physician(s) in order to decide if catheter ablation is right for you.
For over a century, a leader in patient care, medical education and research, with expertise in virtually every specialty of medicine and surgery.
About BWH