Brigham and Women’s Hospital (BWH) is a leader in using state-of-the-art robotics to improve bladder cancer outcomes. This advanced technology’s potential to shorten patient recovery time, combined with the unparalleled experience of our urologic oncology surgical staff, is motivating more of our patients to consider robotic cystectomy.
What is a radical cystectomy?
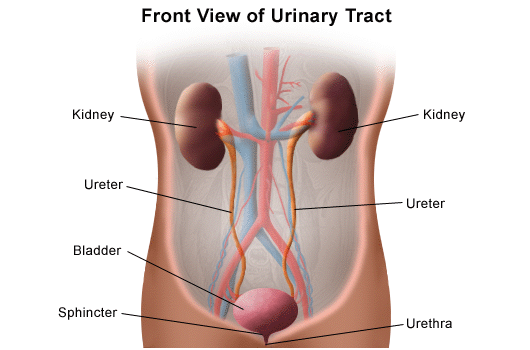
Radical cystectomy, the preferred treatment for muscle-invasive bladder cancer, is the complete removal of the bladder, prostate, seminal vesicles and surrounding tissues in men. In women, it connotes the removal of the bladder, uterus, ovaries and part of the vagina, if necessary. After the bladder is removed, an alternative form of urinary diversion is constructed.
What is a robotic-assisted radical cystectomy?
Robotic radical cystectomy uses a combination of high-definition 3D magnification, robotic technology and miniature instruments to enhance a urologic surgeon’s skills when removing a cancerous bladder.
Open radical cystectomy requires one large incision and retraction to accommodate human hands. However, only tiny incisions in the abdomen are required for the slender robotic arms and tiny surgical tools used in a robot-assisted radical cystectomy and other robotic urologic procedures. Patients will also require another small incision - yet somewhat larger than those needed for the robotic arms - that is required to remove the cancerous bladder and to construct the urinary diversion.
The da Vinci robot has four available arms – one equipped with a high definition 3-D magnification camera, two that act as the surgeon’s arms and a fourth arm that is used for holding back tissue. The surgeon remotely guides the robotic arms while seated at the console, located a short distance away from the patient. These smooth and effortless movements, along with the wristed capabilities of the robotic arms, are the most significant advantages that robotic surgery has over traditional minimally invasive surgical procedures.
What are the benefits of a robotic radical cystectomy?
Robotic surgery’s miniaturization, increased range of motion, enhanced vision and mechanical precision offer significant benefits for radical cystectomy patients, including:
- Less blood loss
- Less risk of needing blood transfusions
- Less post-surgical pain and need for post-operative narcotics
- Quicker recovery and return to normal activities
- Less scarring
Who performs robot-assisted cystectomies at BWH?
Adam S. Kibel, MD, and Steven Lee Chang, MD, MS, represent the robotic urology program at BWH, one of the largest robotic surgery practices in New England. Dr. Kibel, Chief of Urology, has specialized in minimally invasive surgery for urologic cancer for over 15 years. He is one of the most experienced robotic surgeons in New England and one of the most respected cancer surgeons in the country. He has lectured and published widely on the techniques and outcomes of robotic-assisted prostatectomy, partial nephrectomy, and cystectomy.
Dr. Chang completed a fellowship in urologic oncology at Stanford University Medical Center, with an emphasis on minimally invasive surgery. As a result, Dr. Chang employs robotic surgery for nearly all his patients with cancer of the kidney, prostate, or bladder. Dr. Chang frequently lectures on robotic urologic surgery and actively conducts research focused on optimizing robotic techniques and outcomes.
How can I learn more about robotic cystectomy?
If you would like to schedule a consultation with our surgeons, please call the Patient Referral Service - staffed 8am-5:30pm, Monday through Friday - at 1-800-294-9999, or fill out an online request form.