Many aspects of the obstetric management of a twin pregnancy are different than for a singleton pregnancy. Therefore, the maternal-fetal medicine specialists at Brigham and Women’s Hospital (BWH) compiled the following guidelines for the obstetric care of women with twin pregnancies. These guidelines are based on current research, professional society guidelines and the combined knowledge and experience of BWH’s maternal-fetal medicine specialists.
Printable Diagram of the Classification of Identical Twins
Uncomplicated Twin Pregnancy Recommended Timing of Office Visits
|
TWIN CLASSIFICATION |
STARTING AT |
OFFICE VISIT |
|
Dichorionic-Diamniotic (Di-Di) |
|
|
|
Monochorionic-Diamniotic (Mo-Di) |
|
|
|
Monochorionic-Monoamniotic (Mo-Mo) |
|
|
Click here for an illustrated and printable diagram of the classification of identical twins that you can share with your patient.
Below are imaging protocol recommendations adapted from the executive summary on fetal imaging published in the American Journal of Obstetrics & Gynecology in May 2014.*
|
INDICATION |
TIMING |
COMMENT |
|
Pregnancy dating |
First trimester |
|
|
Determination of chorionicity |
First trimester |
|
|
Assessment of nuchal translucency |
10-13 weeks |
|
|
Anatomic survey and placental evaluation |
Second trimester |
|
|
Follow up for Di-Di twins |
Starting at 24 weeks |
|
|
Follow up for Mo-Di twins |
Starting at 16 weeks |
|
|
Amniotic fluid evaluation |
As indicated |
|
|
Doppler scan |
As indicated |
|
* Reddy, UM, Abuhamad AZ, Levine D, Saade GR for the Fetal Imaging Workshop Invited Participants. Fetal imaging: Executive Summary of a Joint Eunice Kennedy Shriver National Institute of Child Health and Human Development, Society for Maternal-Fetal Medicine, American Institute of Ultrasound in Medicine, American College of Obstetricians and Gynecologists, American College of Radiology, Society for Pediatric Radiology, and Society of Radiologists in Ultrasound Fetal Imaging Workshop. Am J Obstet Gynecol 2014; 210 (5): 387-397.
A woman carrying twins has unique nutritional needs, especially for additional calories. Because the patient most often experiences early satiety and loss of appetite, we recommend a consult with a nutritionist to address this and other issues.
Below are the Institute of Medicine’s recommendations for weight gain while carrying twins.
|
PRE-PREGNANCY BMI BODY MASS INDEX (Kg/M2) |
RECOMMENDED WEIGHT GAIN |
|
<18.5 (underweight) |
No recommendation due to insufficient data. |
|
18.5-24.9 (normal weight) |
37-54 pounds or 16.8-24.5 kilograms |
|
25.0-29.9 (overweight) |
31-50 pounds or 14.1-22.7 kilograms |
|
≥30.0 (obese) |
25-42 pounds or 11.4-19.1 kilograms |
All women carrying twins — regardless of age — are candidates for routine aneuploidy screening. For dizygotic twins, there is a higher probability that one or more of the fetuses will have a trisomy, resulting in a higher overall risk to the pregnancy.
The incidence of congenital anomalies is 3-5 fold higher in monozygotic twins than in singletons or dizygotic twins; thus, we stress the importance of an early anatomy ultrasound. The concordance rate of major congenital malformations is approximately 20% in monozygotic twins.
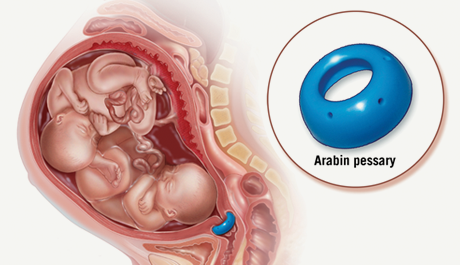
** Romero R, Nicolaides K, Conde-Agudelo A, Tabor A, O'Brien JM, Cetingoz E, Da Fonseca E, Creasy GW, Klein K, Rode L, Soma-Pillay P, Fusey S, Cam C, Alfirevic Z, Hassan SS Vaginal progesterone in women with an asymptomatic sonographic short cervix in the midtrimester decreases preterm delivery and neonatal morbidity: a systematic review and metaanalysis of individual patient data.
Am J Obstet Gynecol. 2012;206(2):124.e1.
Discordant fetal growth is defined as a 20% difference in the estimated fetal weight between the larger and the smaller twin. Those pregnancies with discordant growth and at least one growth-restricted fetus have been associated with a 7.7 fold increased risk of major neonatal morbidity. Thus, pregnancies affected by twin growth discordance should have closer surveillance.
It is common for a twin pregnancy to undergo spontaneous reduction in the first trimester. In the second trimester, up to 5% of twins undergo death of one or more fetuses.
Following the demise of one twin after 14 weeks, the risk of demise of the co-twin is 12-15% in a monochorionic pregnancy and 3-4% in a dichorionic pregnancy. The risk of neurologic abnormality is greater in monochorionic twins (18-26%) than dichorionic twins (1-2 %).***
Immediate delivery after the demise of a twin in the late second or early third trimester has not been shown to be of benefit for the other twin.
The surveillance and delivery recommendations should be individualized, but generally, in the absence of any other complications, delivery before 34 weeks is not recommended.
*** Ong SS, Zamora J, Khan KS, Kilby MD. Prognosis for the co-twin following single-twin death: a systematic review. BJOG. 2006 Sep;113(9):992-8. Epub 2006 Aug 10.
Hillman SC, Morris RK, Kilby MD. Co-twin prognosis after single fetal death: a systematic review and meta-analysis.
Obstet Gynecol. 2011 Oct;118(4):928-40. doi: 10.1097/AOG.0b013e31822f129d.
In addition to a woman’s routine care from her obstetrician, consultation with and additional care from a maternal-fetal medicine specialist is recommended in different cases
The maternal-fetal medicine specialists at BWH are always happy to answer questions or provide a consult. You can send a question via email or call us directly.
Carolina Bibbo:
cbibbo@partners.org
Phone: (617) 732-5452
There is no role in antepartum fetal surveillance for uncomplicated Di-Di or Mo-Di twin gestations. Antepartum fetal surveillance is reserved for twin pregnancies complicated by maternal or fetal disorders that require antepartum testing, such as fetal growth restriction.
We are happy to respond to general questions about twin pregnancies. Please use our online form to send us your twin pregnancy question, and one of our maternal-fetal medicine specialists will respond. Please note that your question will be emailed and responded through a private and secure system.
For over a century, a leader in patient care, medical education and research, with expertise in virtually every specialty of medicine and surgery.
About BWH